What Is Pelvic Congestion Syndrome
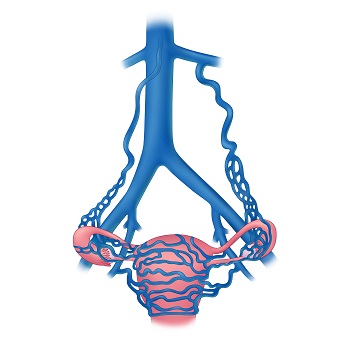
Pelvic congestion syndrome, also called pelvic venous congestion, falls under a broader range of pelvic venous disorders which are a known, but often unrecognized cause of chronic pelvic pain. Varicose pelvic veins develop when the valves in veins are not working correctly, or occasionally when critical deeper veins are obstructed, causing blood to pool and distend pelvic veins.
Healthy veins return blood to the heart through one-way valves, allowing blood to travel toward the heart.
Congested veins have weakened valves, allowing blood to flow backward and distend pelvic veins.
Occasionally, increased pressure inside pelvic veins may be the result of an obstruction in the major veins draining the pelvis.
Commonly Recognized Associations
Although the causes of pelvic venous congestion are complex and poorly understood, a few commonly recognized associations include:
• Family history of venous disease
• Multiple pregnancies
• Estrogen
• Pelvic or renal vein compression
It is estimated that 30% of patients with chronic pelvic pain of an unknown cause actually suffer from a symptomatic pelvic venous disorder.
What Are the Symptoms of Pelvic Congestion Syndrome?
Typical symptoms of pelvic congestion include:
• Dull achiness and/or heaviness in the pelvis, often made worse by prolonged standing
• Bloating sensation
• Pain in the lower back
• Visible varicose veins on the buttocks, vulva, and upper thighs
• Painful menstrual cycle with referred pain in the legs
• Increase urination frequency
• Pain during and after intercourse
How Is Pelvic Venous Congestion Diagnosed?
Unfortunately, pelvic venous congestion often goes unrecognized and untreated. Symptoms, physical exam and ultrasound findings have a high combined predictive value in diagnosing pelvic venous disorders. The ability of duplex ultrasound (DUS) to image realtime makes it an important tool in the evaluation of possible pelvic venous congestion.
Because there are many other potential causes of chronic pelvic pain, medical professionals may conduct multiple exams and tests including:
• Pelvic exam
• Pelvic duplex ultrasound
• CT or MRI scan
• Laparoscopy
What are the Treatment Options?
Once a patient is diagnosed with pelvic venous congestion, it can often be successfully treated with a minimally invasive procedure called embolization. Pelvic venous embolization requires little or no downtime and is performed in an outpatient setting. Occasionally, a compressed iliac vein may contribute to venous congestion and a stent may be indicated to help restore normal flow. Embolization requires little or no downtime, is performed as an outpatient, and is minimally invasive but highly effective. After treatment, patients are typically able to return to most routine activities the same day.
Treatment Tips
• Wear comfortable clothing to the procedure
• Eat a light meal the evening before your procedure
• Don’t eat or drink less than 6 hours before treatment, unless directed by your doctor
• Over-the-counter pain medication is typically all that is needed after the procedure
• While recovering, stay active but avoid heavy lifting
• Reach out to your treating doctor with any questions or concerns
Learn more at
ivein.com
Resources
Black, C.M. and Dillavou, E.D. “Endovascular Treatment for Pelvic Venous Congestion Syndrome.” Master
Techniques in Surgery – Vascular Surgery: Hybrid, Venous, Dialysis Access, Thoracic Outlet and Lower Extremity
Procedures. Ed. R. Clement Darling III, Ed. C. Keith Ozaki. Philadelphia. Wolters Kuwer, 2016, pp. 127-134. Print.
https://www.ivein.com/conditions/pelvic-congestion-syndrome/
https://stanfordhealthcare.org/medical-conditions/womens-health/pelvic-congestion.html
https://thewhiteleyclinic.co.uk/wp-content/uploads/The-Impact-of-Pelvic-Congestion-Syndrome-Report.pdf