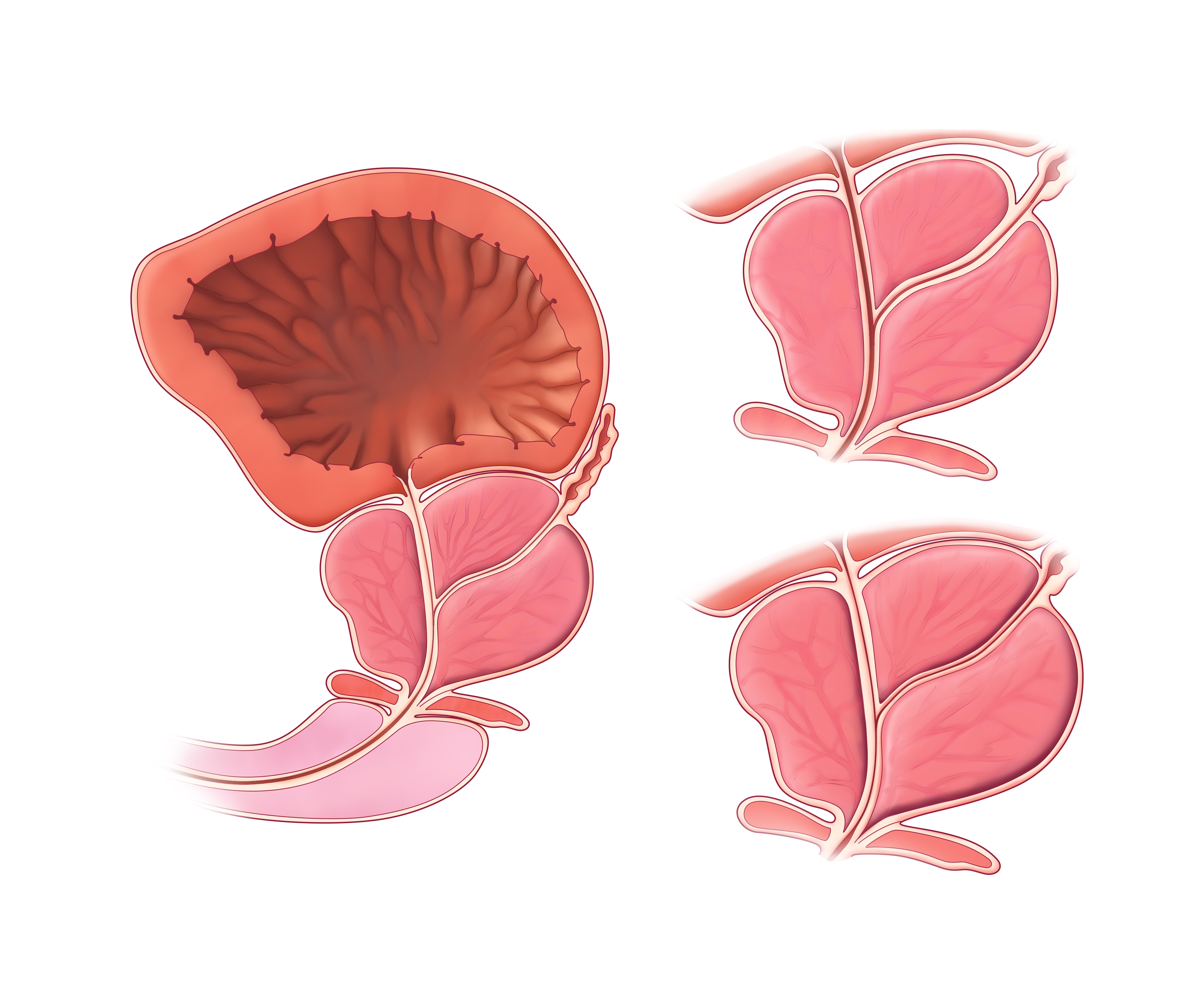
What is Benign Prostatic Hyperplasia (BPH)?
BPH is a condition where the prostate gland, located just below the bladder and surrounding the urethra, grows larger with age. This enlargement is common—about half of men over 50 and up to 80% of men over 80 experience it. While not cancerous, an enlarged prostate can press on the urethra, leading to urinary symptoms that range from mild to disruptive. These may include:
- Frequent urination, especially at night (nocturia)
- Trouble starting or maintaining a urine stream
- Weak or interrupted urine flow
- A feeling of incomplete bladder emptying
- Urgency or discomfort during urination
In some cases, untreated BPH can lead to complications like urinary tract infections, bladder stones, or kidney issues. If medications or lifestyle changes aren’t providing relief, or if you prefer to avoid traditional surgery, treatments like PAE may be considered.


